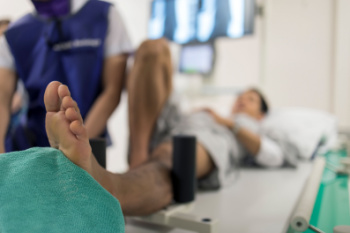
An ankle fracture occurs when one or more of the bones surrounding the ankle joint break, typically due to trauma or excessive force. Diagnosis of an ankle fracture begins with a thorough physical examination by a podiatrist, including assessment of symptoms and a review of the injury's circumstances. Imaging tests such as X-rays are then used to confirm the diagnosis and determine the extent of the fracture. Symptoms of an ankle fracture often include severe pain, swelling, bruising, and difficulty bearing weight on the affected foot. In some cases, the ankle may appear deformed or out of alignment. Additionally, individuals may experience a limited range of motion and tenderness to touch surrounding the ankle joint. Prompt diagnosis and appropriate treatment are essential in managing ankle fractures effectively. If you have broken your ankle, it is suggested that you consult a podiatrist who can discuss which treatment options are right for you.
Broken ankles need immediate treatment. If you are seeking treatment, contact Dean Kim, DPM from Greater Texas Foot & Ankle Specialist. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
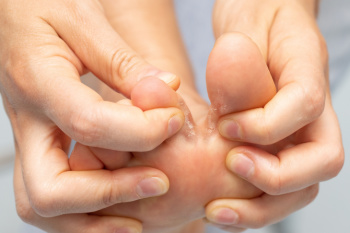
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our office located in Frisco, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.